General examination in open angle glaucoma
|
||
|
In the examination, the examiner may ask you to examine a patient with known open angle glaucoma. You need to look for :
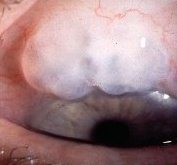
operation the second trabeculectomy may be found more temporally. Iridectomy is usually present. Poor drainage is suggested by an absence of bleb or a dome-shaped vascularized bleb caused by subconjunctival fibrosis. Occasionally, you may encounter patients who had Scheie procedure for aqueous drainage. This full-thickness filtering surgery. The anterior chamber is opened to the subconjunctival space. Uveal tissue is visible at the sclerotomy site. This procedure is now out-dated. Other physical signs associated with glaucoma treatment include:
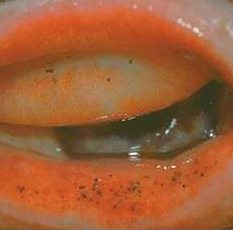
This can be easily missed unless you evert the lower lid which it is most commonly seen.
The severity of the glaucoma is graded according to the
loss of neural tissue best seen at the optic disc.
|
Questions:
1. What are the advantages and disadvantages between limbal
based and fornix based conjunctival flap in trabeculectomy?