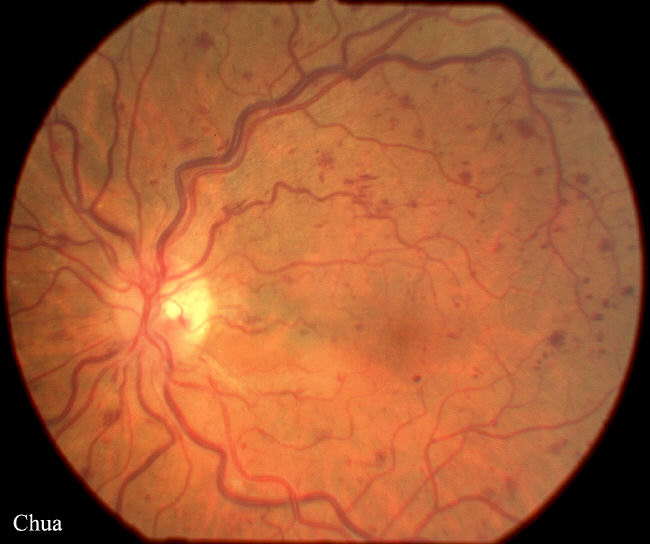
| History: This 75 year-old man with a history of hypertension complained of a two-day history of blurred right vision. He was otherwise in good health. His vision was 6/12 in the right eye and 6/6 in the left eye with normal intraocular pressures. There was no relative afferent pupillary defect. Fundoscopy revealed dilated retinal veins and widespread multiple blot haemorrhages. The diagnosis was non-ischaemic central retinal vein occlusion. The blood tests for full blood counts, ESR and glucose were normal. He was revealed six weeks later and the vision improved to 6/9. Occasionally non-ischaemic central retinal vein occlusion can progress to ischaemic central retinal vein occlusion and it is important to review the patient within the first two months for any such progression. The main cause of visual loss in central retinal vein occlusion are macular oedema and neovascularization which can lead to neovascular glaucoma. The macular oedema does not respond to focal laser. Panphotocoagulation is used to treat retinal neovascularization and prevent the development of neovascular glaucoma. | |||
 |
|||
|