Figure1 |
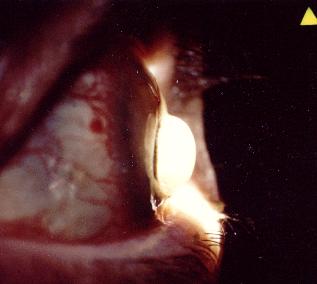
Figure 2 |
Eyelids and Anterior Segment: Case three

Figure1 |

Figure 2 |
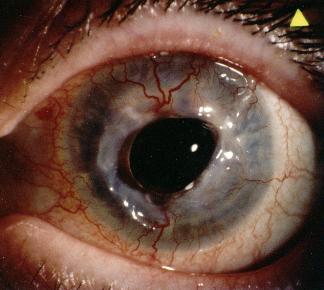
This 75 year old woman with a long-standing history of rheumatoid arthritis presented to the eye casualty with a sudden onset loss of her right vision. She was known to suffer from severe dry eyes and there was no history of trauma. On examination, her visual acuity was light perception in the right eye and 6/18 in the left. The slit-lamp appearance of the right eye is shown in
Figure 1 & 2.a. What is the diagnosis?
The pictures show a right central corneal perforation and the perforation is plugged by the vitreous. The diagnosis is keratolysis secondary to rheumatoid arthritis.Keratolysis is a fulminant process which involves acute melting of clear corneal stroma resulting in severe thinning, with descemetocele formation or perforation. It is often associated with scleromalacia perforans.
b. Is corneal graft useful in this patient?Corneal graft in keratolysis is usually disappointing because the tissue around the perforation is disorganized making suturing unstable. The presence of dry eye also impairs healing.c. What other ocular complications may occur in patient with rheumatoid
A tectonic graft was performed on this patient. Unfortunately, she developed recurrent perforation and evisceration was eventually performed.
arthritis?Ocular complications of rheumatoid arthritis include:
- keratoconjunctivitis from secondary Sjogren's syndrome
- scleritis
necrotizing anterior scleritis with inflammation
necrotizing anterior scleritis without inflammation (scleromalacia perforans)
non-necrotizing anterior scleritis
posterior scleritis- corneal problems
keratolysis
sclerosing keratitis
acute stromal keratitis
peripheral guttering- drug-induced
steroid causing glaucoma and posterior subcapsular cataract
hydroxychloroquine causing vortex keratopathy, cataract ( usually of
no visual consequence) and bull eye maculopathy.
Click here for questions Click here for the main page Click here for MRCOphth/FRCS tutorials