A Short Guide to Ophthalmology as a Career in the UKIntroductionOphthalmology is unique amongst medical specialties. The eye, its surrounding structures and the visual pathway may be affected by a great variety of clinical conditions. Their successful management depends on the ophthalmologist combining the diagnostic and therapeutic abilities of a physician and technical skills of a microsurgeon with an understanding of the whole patient. One of the fundamental properties of the eye is that many of its components are transparent. This enables the details of its structure and abnormalities to be observed directly, in a manner not possible for many other parts of the human body. Disorders of the eye and visual system commonly cause reduction in vision. It is therefore not surprising that one of the major rewards of the profession is to be able to restore sight, for example by removing a cataract. In recent years, ophthalmology has rapidly incorporated new technologies into daily practice. Developments in optical instrumentation have improved the clarity and magnification with which the components of the eye can be observed and imaged. A variety of lasers are now used to perform out-patient procedures which previously required admission to hospital. Improvements in microsurgical instrumentation have led to the development of procedures not considered possible as little as a decade ago. The Role of the Ophthalmolgist The ophthalmologist is both physician and surgeon for conditions occurring in and around the eye and the visual pathways. The majority of patients are seen in the out-patient department and many require follow-up of an ongoing condition. A minority of patients require laser procedures or surgery, of which an increasing proportion is being performed under local anaesthesia and as a daycase. The surgical work of the general ophthalmologist may include cataract extraction, squint and glaucoma surgery, retinal, oculoplastic and nasolacrimal surgery. Many consultant ophthalmologists have an area of particular interest and expertise for which they may hold special clinics (Table 1). Emergencies may be seen first by a general casualty officer but in large departments a separate Eye Casualty department is staffed by junior ophthalmologists or nurse practitioners. Patients present with conditions ranging from a simple foreign body on the eye to chemical burns, angle-closure glaucoma or retinal detachment. The eye and its surrounding structures can be involved in systemic and local disease. There is therefore close cooperation with many other specialists, including diabetologists, rheumatologists, neurologists, neurosurgeons, ENT and maxillofacial surgeons, plastic surgeons, paediatricians and geneticists. Interdisciplinary working Ophthalmologists perform most of their work in the eye department of the main hospital, and some hold out-patient sessions at peripheral clinics. Other professionals also play an important role in the care of ophthalmic patients, and teamwork is essential to ophthalmic practice. Ophthalmic Nurses have training and experience in ophthalmology, and provide specialist support for eye clinics, wards and operating theatres. Some also undergo further training to become nurse practitioners. Orthoptists undergo professional training to become expert in problems of ocular movement, binocular vision and children's sight. They may work as part of the team within the eye unit itself, or independently as community orthoptists. Optometrists also undergo professional training. Many practice in the High Street, refracting patients and prescribing and dispensing spectacles. Some work part-time or full-time within the Hospital Eye Service, where they provide specialist services such as the fitting of complex contact lenses and low vision aids. Ocular Prosthetists are responsible for the manufacture and fitting of ocular and oculofacial prostheses when tissue has been lost through trauma or surgery. Ophthalmic Photographers use sophisticated equipment to photograph the face, eyelids, outer eye, and retina. Photographic and video techniques are important in the diagnosis and monitoring of many ophthalmic disorders. Electrophysiologists mainly work in teaching hospital eye departments and provide electrodiagnostic and monitoring services for patients with suspected or established inherited retinal diseases or visual pathway disorders. Training in ophthalmology is divided into two main parts (Figure 1). Basic specialist training (BST) as a Senior House Officer lasts a minimum of 2 years. Higher specialist training (HST) as a Specialist Registrar (SpR) lasts 4 1/2 years. BST and HST are supervised by deanery Specialty Training Committees (STCs) and by the Training Committee of the Royal College of Ophthalmologists. The 'Directory of Training Posts in Ophthalmology' published by the Royal College of Ophthalmologists lists details of all eye departments and posts in the UK which are recognised for training. Teaching hospitals tend to have large eye departments with more consultants and trainees in HST. They offer subspecialty services and training, with opportunities for research. District general hospitals tend to have smaller departments with large clinical loads offering a wide variety of experience, both in the clinic and the operating theatre. Prior to entering Ophthalmology Ophthalmology is a highly competitive specialty. If as a medical student you are seriously considering a career in ophthalmology, it is worthwhile thinking how you might enhance your curriculum vitae. You may like to include ophthalmology in one of your elective or optional periods. Clinical medical students are eligible to enter the Duke-Elder Prize in Ophthalmology, which is a national competitive MCQ examination run by the Royal College of Ophthalmologists. Following qualification, preregistration house officer posts must be completed. Prior to entering ophthalmology, some trainees spend six months or more in allied specialties, such as accident and emergency, general medicine, neurology, neurosurgery, plastic surgery and other subjects appropriate for General Professional Training (GPT). Basic Specialist Training (BST) At least two years are spent in BST as an SHO. During BST, the trainee should acquire the general clinical skills of an ophthalmologist, and have a basic knowledge of the conditions covered by the specialty. There is an average of two theatre sessions per week, during which the trainee should master the commonly-performed procedures, and assist at more complex operations. Basic surgical trainees may want to become involved in clinical research projects. Many SHO posts in ophthalmology are suitable as General Professional Training (GPT) for doctors who wish eventually to enter another specialty or have yet to choose a career. The arrangements for postgraduate examinations in ophthalmology are set out in Table 2. Higher Specialist Training (HST) Competition for entry to the Specialist Registrar Grade is considerable. All applicants must have passed the MRCOphth (new regulations). STC interview panels also look for other attributes such as participation in research, presentations at meetings, publications in journals, and other more individual achievements. During the 4 1/2 year period of HST, trainees will increase the depth of their knowledge, and learn specialist surgical skills according to a curriculum set by the College. More time is spent in both general and specialist clinics, and there is an average of three theatre and laser sessions per week. Regular assessment of trainees' progress is undertaken by the trainers and an annual STC assessment panel. Before, during or after HST, one to three years may be taken out in a full-time research post in an academic department of ophthalmology, after which a thesis may be submitted for an MD or PhD degree. It may be possible to organise additional work abroad for shorter periods of time, for example in third world countries. Throughout HST all entrants to the SpR grade are expected to prepare for the Fellowship Assessment. This consists of written reports on cases personally managed by the candidate during HST. The cases should reflect not only the breadth of the candidate's training but also experience gained in the management of problems and familiarity with relevant scientific literature. The case book will be presented during the final stages of training and will be assessed at a viva voce interview by three examiners. Successful performance in both the Fellowship Assessment and annual STC assessments leads to the award of the FRCOphth (new regulations) and the Certificate of Completion of Specialist Training (CCST). The trainee is then eligible to apply for consultant posts in the UK, or equivalent posts in Europe and a number of other countries. Flexible Training Trainees unable to work full-time for family reasons may undertake an equivalent training programme, but over a longer period. Local arrangements are made through the Regional Postgraduate Dean. Medical Ophthalmology This is a distinct branch of ophthalmology for which specialist training can be undertaken and qualifications obtained. Medical ophthalmologists generally do not perform surgery. Their sphere of interest embraces diabetes and endocrinology, vascular disease of the eye, uveitis, AIDS, the ramifications of dermatological and rheumatological disorders, paediatric ophthalmology and genetics, and neuro-ophthalmology. Career Grade Ophthalmologists The majority of trainees aim to become consultants, for which the FRCOphth (or equivalent) and CCST are essential. There are approximately 760 ophthalmic consultant posts in the UK. Consultants are responsible for all the patients in their care, and for supervising and training junior doctors. Posts may be full-time, part-time or job-share. There are numerous SpRs applying for each consultant job and the specialty is very competitive. Other career options For trainees who are unable, or do not wish, to become consultants but want to continue a career in ophthalmology, there are other options available, depending upon experience, within the non-consultant career grades (NCCGs). Clinical assistants are individuals who have some basic training in ophthalmology, and usually work in the outpatient department on a sessional basis. The posts are particularly suitable for those wanting to work part-time, or to combine an interest in ophthalmology with a commitment in another specialty, such as general practice. To obtain a staff grade post, completion of basic specialist training is required. The type of work performed is dependent upon the individual's interests and experience. Posts may be full-time or part-time. An associate specialist is a similar appointment made on a personal basis to an individual with appropriate qualifications and training who has spent a number of years as a staff grade ophthalmologist. They commonly have a subspecialty interest. Academic Ophthalmologists There are many academic departments in ophthalmology throughout the UK which are staffed by Professors, Senior Lecturers and Clinical Lecturers. Professors and Senior Lecturers have honorary consultant contracts and Lecturers have honorary SpR contracts. Ophthalmologists wishing to pursue an academic career would normally be required to have a higher degree and should seek advice early on clinical training requirements. Summary Ophthalmology is a specialty with something for everybody. It is typified by variety not only in the patients cared for and the types of conditions treated, but also the techniques used and operations performed. The professional satisfaction is high as we are able to offer most patients effective treatment. As the specialty is so popular, there is intense competition for training posts, but great scope for those committed to a career in ophthalmology. Additional Documents The College will supply additional information about curricula of training, examinations, training of overseas doctors and other topics on request. Useful Contacts Your local Department of Ophthalmology Your Regional Postgraduate Dean The Royal College of Ophthalmologists
The British Medical Association
The General Medical Council
TABLE 1 - OPHTHALMIC SUBSPECIALTIES
TABLE 2 - EXAMINATIONS OF THE ROYAL COLLEGE OF OPHTHALMOLOGISTS
D = Diploma
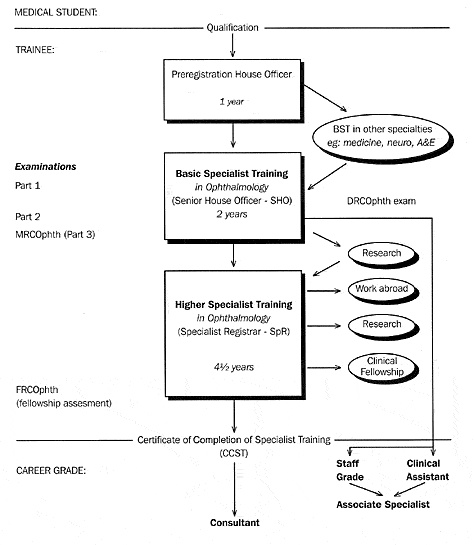
** Although experience in approved posts is not required for examination purposes it should be noted that candidates seeking Higher Specialist Training posts and Certificates of Completion of Specialist Training are required to have spent the requisite time in posts which have been inspected and approved by The Royal College of Ophthalmologists. For further information on this point, please contact the College's Education and Training Department. Figure 1 Career structure on ophthalmology for full-time trainees. The typical times at which examinations are taken are shown on the left; and the various options possible at different stages are shown on the right.
|
|||||||||||||||||||||||||||||||||||||||||||||