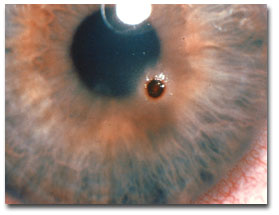
| Essential topics/experience:
To have become familiar with the following: i. Superficial ocular trauma: including assessment and treatment of foreign bodies, abrasions and minor lid lacerations. ii. Severe blunt ocular injury: management of hyphaema; recognition and initial management of more severe injury. iii. Severe orbital injury: recognition and initial management of blow-out fracture, optic nerve compression. iv. Penetrating ocular injury: recognition and initial care of corneal and scleral wounds; recognition of aqueous leakage and tissue prolapse. v. Retained intraocular foreign body: anticipation from history; confirmation by X-Ray and CT scan. vi. Sudden painless loss of vision: recognition of retinal arterial occlusion, central retinal vein occlusion, acute ischaemic optic neuropathy, optic neuritis; urgency of treatment. vii. Severe intraocular infection: recognition and initial investigation and management of hypopyon. viii. Acute angle closure glaucoma: recognition and acute reduction of intraocular pressure. ix. Liaison: with radiological department, microbiologists, ENT, faciomaxillary surgeons. Practical skills:
i. Removal of superficial foreign bodies. ii. Corneal epithelial debridement. iii. Repair of minor conjunctival/lid lacerations. iv. YAG iridotomy. Background theory/principles:
i. Eye protection and prevention of injury. ii. Lateral canthotomy and inferior cantholysis for retrobulbar haemorrhage. iii. Chemical/alkali burns of the conjunctiva and cornea. iv. Drug penetration into the eye and vitreous. v. Use of intravitreal antibiotics, including dosage and potential complications. |
|||
|